Fact sheet 01-2017
Telerehabilitation
Telerehabilitation (TR) involves providing rehabilitation through information and communication technology, regardless of the patient’s geographical location (1). As traditional rehabilitation, TR consists in patient assessment, clarification of goals, patient-tailored therapies, including exercise, as well interdisciplinary collaboration between different health professionals.
There are three categories of TR: image-based TR, sensor-based TR and use of virtual technologies (4, 5). TR can be performed via videoconferencing where patients and health professionals have real-time contacts, via recording of video sessions, or via automated algorithms which guide the patients through an exercise programme (6). Sensors measuring glucose levels, blood pressure, oxygen saturation or physical activity can provide an overview of the evolution of the patient’s health status without the need to visit a health institution (3, 7).
Various studies have shown that TR can have similar effects to those of traditional rehabilitation (3).
Advantages of telerehabilitation
The use of TR can eliminate practical barriers, such as difficult weather conditions and long travel distances. Differences between municipalities can be reduced by the provision of specialised rehabilitation where this is not available (3, 8). TR allows for more frequent exercise sessions than traditional centre-based rehabilitation programmes, which are often provided 1-2 times a week (3, 4). Furthermore, the technology can encourage exercise regularity through tailored motivational messages, which can prevent dropout during holiday periods. TR can be conducted individually or in groups. Interactive features and gamification elements can create group affiliation and increase training motivation (8). Rehabilitation in the home environment can also support long-term exercise maintenance (9).
Experience with telerehabilitation in Norway
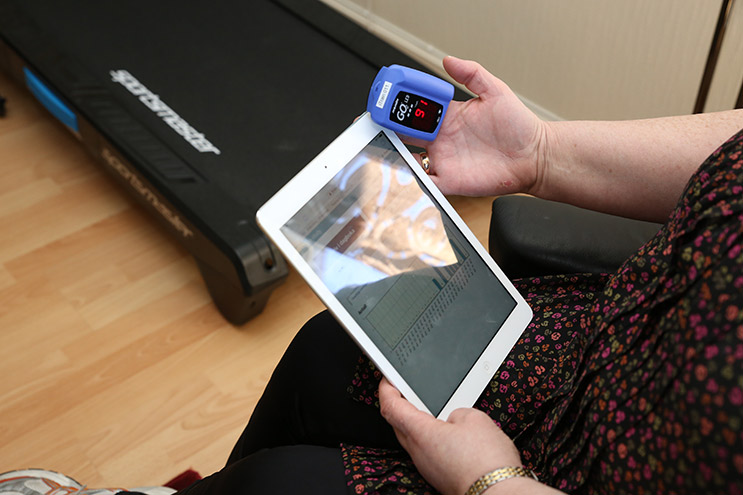
There are few examples of use of TR in Norway. A pilot study in which a two-year TR intervention was offered to patients with COPD showed that TR is feasible and that patients were satisfied (8). Participants trained on a treadmill at home, registered symptoms and oxygen saturation in a website available on a tablet, and received weekly follow-up by a physiotherapist via videoconferencing. Despite deterioration in COPD is expected over time, the participants maintained their physical capacity, health status and quality of life. The number of hospitalisations and outpatient visits were also reduced (10). An international multicentre randomised controlled trial is currently being conducted . This study will provide evidence on whether TR is a cost-effective strategy for follow-up of patients with COPD (11).
Challenges of telerehabilitation
Adopting TR in clinical practice requires organisation changes which may be challenging. So far, only few telemedicine interventions have evolved beyond the pilot phase. There are currently no strategic plans or referral schemes which encourage large-scale implementation of TR in Norway. Moreover, there is still little knowledge on which patients woud benefit most from TR (3). Computer literacy among the users may affect adherence, and the technology must be available and affordable to those who want to make use of TR (12). The cost-effectiveness of TR remains still unknown. Future studies should therefore evaluate organisational and economic effects of TR.
References
- Rosen MJ. Telerehabilitation. NeuroRehabilitation. 1999;12(1):11-26.
- Helse- og omsorgsdepartementet. Forskrift om habilitering og rehabilitering, individuell plan og koordinator Lovdata.no2012 [Tilgjengelig fra: https://lovdata.no/dokument/SF/forskrift/2011-12-16-1256/KAPITTEL_2#§3.
- Langberg H, Lindahl MP, Kidholm K, Dinesen B. Telerehabilitering. Ugeskrift for Læger. 2014;176(10):944-7.
- Theodoros D, Russell T. Telerehabilitation: current perspectives. In: Latifi R, editor. Current principles and practices of telemedicine and e-Health: IOS Press; 2008. p. 191-210.
- Russell T. Physical rehabilitation using telemedicine. J Telemed Telecare. 2007;13(5):217-20.
- Cherney LR, van Vuuren S. Telerehabilitation, Virtual Therapists, and Acquired Neurologic Speech and Language Disorders. Semin Speech Lang. 2012;33(3):243-57.
- Tabak M, Brusse-Keizer M, van der Valk P, Hermens H, Vollenbroek-Hutten M. A telehealth program for self-management of COPD exacerbations and promotion of an active lifestyle: a pilot randomized controlled trial. Int J Chron Obstruct Pulmon Dis. 2014;9:935.
- Hoaas H, Andreassen H, Lien L, Hjalmarsen A, Zanaboni P. Adherence and factors affecting satisfaction in long-term telerehabilitation for patients with chronic obstructive pulmonary disease: a mixed methods study. BMC Med Inform Decis Mak. 2016;16(1):26.
- Holland AE, Mahal A, Hill CJ, Lee AL, Burge AT, Moore R, et al. Benefits and costs of home-based pulmonary rehabilitation in chronic obstructive pulmonary disease-a multi-centre randomised controlled equivalence trial. BMC Pulm Med. 2013;13(1):1.
- Zanaboni P, Hoaas H, Lien LA, Hjalmarsen A, Wootton R. Long-term exercise maintenance in COPD via telerehabilitation: A two-year pilot study. J Telemed Telecare. 2016;0(0):1-9.
- Zanaboni P, Dinesen B, Hjalmarsen A, Hoaas H, Holland AE, Oliveira CC, et al. Long-term integrated telerehabilitation of COPD Patients: a multicentre randomised controlled trial (iTrain). BMC Pulm Med. 2016;16(1):126.
- O’Connor S, Hanlon P, O’Donnell CA, Garcia S, Glanville J, Mair FS. Understanding factors affecting patient and public engagement and recruitment to digital health interventions: a systematic review of qualitative studies. BMC Med Inform Decis Mak. 2016;16(1):120.